1. Understanding the Purpose of a Colonoscopy
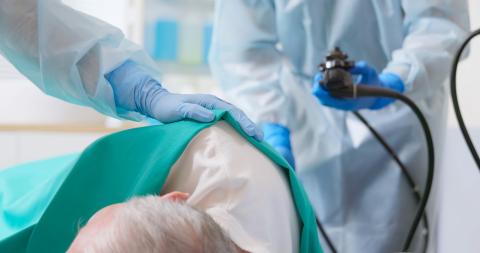
A colonoscopy is a diagnostic procedure that allows doctors to examine the lining of the colon and rectum using a flexible tube with a camera, called a colonoscope. Understanding the purpose of the procedure is essential before scheduling it, as it informs patients about the benefits, potential risks, and expected outcomes. Colonoscopies are primarily recommended for the early detection of colon cancer, polyps, or other abnormalities, especially in individuals over 45 or those with a family history of colorectal disease.
Doctors may also recommend colonoscopies for patients experiencing unexplained gastrointestinal symptoms such as persistent diarrhea, rectal bleeding, abdominal pain, or changes in bowel habits. By understanding the purpose of the procedure, patients can set realistic expectations and actively participate in decision-making about their health. Knowing why the test is necessary reduces anxiety and ensures better compliance with pre-procedure instructions.
2. The Key Question: “Why am I getting this colonoscopy?”
While patients often focus on procedural details, the most important question to ask your doctor before a colonoscopy is, “Why am I getting this colonoscopy?” This question encourages a clear explanation of the indication for the procedure, whether it’s routine screening, surveillance due to previous findings, or diagnostic evaluation due to current symptoms.
Understanding the reason helps patients gauge the urgency and frequency of the test. For example, a routine screening colonoscopy may differ in preparation and urgency compared to a procedure aimed at investigating rectal bleeding. By asking this question, patients gain insight into their personal risk profile, the likelihood of finding abnormalities, and potential follow-up procedures. It also allows them to clarify concerns about alternative screening methods, ensuring the chosen approach aligns with their needs and comfort level.
3. Preparation Requirements
Colonoscopy preparation is a crucial aspect of the procedure and often the most challenging part for patients. Proper bowel preparation ensures clear visibility for the doctor and increases the likelihood of detecting polyps or other abnormalities. Preparation typically involves dietary restrictions, such as a clear liquid diet 24–48 hours before the procedure, and the use of prescribed laxatives or cleansing solutions.
Discussing preparation in detail with your doctor is essential. Patients should ask about the exact timing, dosage, and type of laxative recommended, as well as strategies for staying hydrated and managing potential discomfort. Understanding preparation steps helps reduce stress and confusion, ensuring a smoother experience and improving the accuracy of the colonoscopy.
4. Understanding Risks and Complications
Although colonoscopy is generally safe, it is not without potential risks. These can include reactions to sedation, bleeding, perforation of the colon, or infection. Discussing these risks in advance allows patients to weigh the benefits of early detection against the rare possibility of complications.
Doctors can explain risk factors specific to each patient, such as age, medical history, or pre-existing conditions, and recommend additional precautions if necessary. Understanding risks also helps patients recognize warning signs after the procedure, such as prolonged abdominal pain, fever, or rectal bleeding, prompting timely medical attention. Knowledge about potential complications empowers patients to make informed decisions and reduces anxiety about the procedure.
5. Sedation Options and Comfort Measures
Most colonoscopies involve some form of sedation to minimize discomfort and ensure patient cooperation. Discussing sedation options, including conscious sedation or deeper anesthesia, is critical to address patient comfort, safety, and recovery expectations. Patients should ask about side effects, duration of sedation, and recovery time, including when they can safely drive or resume normal activities.
Additionally, understanding comfort measures during the procedure, such as positioning, communication with the doctor, and strategies for reducing anxiety, can improve the overall experience. Clarifying these aspects before the procedure helps patients feel prepared, reduces stress, and encourages adherence to medical advice, ultimately contributing to a successful and effective colonoscopy.
6. Frequency and Timing of Colonoscopies
One of the most important aspects to clarify with your doctor is how often colonoscopies are recommended for you. The frequency depends on factors like age, personal medical history, family history of colon cancer, and previous colonoscopy findings. For average-risk adults, routine screening usually begins at age 45 and continues every ten years if results are normal.
For patients with polyps, inflammatory bowel disease, or a family history of colorectal cancer, doctors may recommend more frequent surveillance, such as every three to five years. Understanding the timing helps patients plan ahead and ensures that colonoscopies are performed when most beneficial. Asking your doctor to explain the reasoning behind the recommended interval also allows you to evaluate risk factors and make informed decisions about your long-term screening schedule.
7. Understanding the Procedure Step by Step
Another key question is asking your doctor to walk you through the colonoscopy procedure itself. Knowing what to expect—from preparation and sedation to insertion of the colonoscope and inspection of the colon lining—can reduce anxiety and make the process feel more manageable.
Doctors often explain that the procedure typically takes 20–60 minutes, during which the doctor can examine the colon and remove polyps if needed. Sedation is used to ensure comfort, and patients usually feel relaxed or sleepy rather than experiencing pain. Post-procedure, recovery may involve minor bloating or cramping, but most people resume normal activities within a day. By asking for a detailed explanation, patients can mentally prepare, which improves cooperation and overall satisfaction with the experience.
8. Possible Findings and Next Steps
It’s essential to ask your doctor about potential findings and what follow-up steps might be required. Polyps, inflammation, bleeding sources, or other abnormalities may be discovered during the colonoscopy. Most polyps are benign, but some can be precancerous, highlighting the importance of early detection and removal.
Understanding possible results helps patients prepare for follow-up procedures, additional testing, or lifestyle changes that may be recommended. Discussing scenarios such as biopsies or polyp removal ensures patients are informed about risks, recovery, and potential implications. This proactive approach reduces uncertainty and allows patients to make informed decisions about their health care.
9. Post-Procedure Care and Recovery
Recovery after a colonoscopy is another crucial topic to discuss. Depending on the type of sedation used, patients may need someone to drive them home and should avoid making important decisions or operating heavy machinery for the rest of the day. Light meals and adequate hydration are recommended, while strenuous activity may be temporarily limited.
Doctors can also advise on managing minor discomforts like bloating, cramping, or mild fatigue. Knowing what to expect during recovery helps patients plan their day, reduces anxiety, and ensures adherence to post-procedure instructions. This guidance is particularly important for older adults or those with underlying health conditions, as tailored recovery recommendations can minimize complications and support a smooth healing process.
10. Risks vs. Benefits in Your Specific Case
Finally, patients should ask their doctor to explain the risks versus benefits of a colonoscopy in their specific context. While colonoscopies are highly effective at detecting and preventing colorectal cancer, individual risk factors, age, and medical history can influence the decision.
Understanding personalized benefits—such as early detection of polyps or prevention of colorectal cancer—is balanced against potential risks, including bleeding, infection, or complications from sedation. Having this conversation ensures patients make an informed choice and feel confident that the procedure is appropriate for them. It also allows for discussion of alternative screening options, if applicable, and reassures patients that their care plan is tailored to their needs.
11. Polyp Detection and Removal
One of the primary reasons for undergoing a colonoscopy is to detect and remove polyps, which are small growths on the lining of the colon. While most polyps are benign, some can develop into cancer over time if left untreated. Doctors often perform polyp removal during the colonoscopy itself, a process known as polypectomy.
Understanding the procedure for polyp removal helps patients feel more prepared and reduces anxiety about potential findings. Polyp removal is usually safe and does not significantly increase recovery time. By detecting and removing polyps early, colonoscopy serves as both a diagnostic and preventive procedure, which underscores the importance of discussing polyp detection with your doctor prior to the test.
12. Biopsy Procedures During Colonoscopy
In addition to visual inspection and polyp removal, colonoscopies allow doctors to perform biopsies. A biopsy involves taking a small tissue sample from the colon lining for laboratory analysis. This can help diagnose conditions such as inflammation, infections, or early-stage cancers.
Knowing that biopsies can be performed during the procedure is important because it allows patients to anticipate the need for follow-up results and potential additional treatment. Doctors typically explain how tissue samples are collected, the associated risks, and the expected timeline for results. Understanding this aspect helps patients feel informed and involved in their care, reducing uncertainty about what might happen during the colonoscopy.
13. Sedation Risks and Safety
Sedation is commonly used during colonoscopy to ensure patient comfort, but it carries potential risks. Depending on the patient’s age, health status, and prior reactions to sedation, doctors may recommend different types or doses of sedatives. Some patients may experience mild side effects, such as drowsiness, nausea, or temporary disorientation, while rare complications can include breathing difficulties or reactions to the medication.
Patients should discuss their medical history, including heart, lung, or liver conditions, with their doctor prior to the procedure. Knowing sedation risks in advance allows patients to take appropriate precautions, arrange for transportation home, and understand recovery expectations. Clear communication with the healthcare team about sedation ensures both safety and comfort during the procedure.
14. Dietary Restrictions Before the Procedure
Proper bowel preparation is critical for an effective colonoscopy, and this requires adherence to dietary restrictions. Doctors usually recommend a clear liquid diet for 24–48 hours before the procedure, avoiding solid foods that could obscure the colon lining. Clear liquids may include water, broth, clear juices, or tea and coffee without milk.
Understanding these dietary requirements and the reasons behind them helps patients comply fully and reduces stress during preparation. Patients should also ask about hydration strategies to avoid dehydration, particularly for those who may have underlying health conditions. Proper preparation maximizes the accuracy of the colonoscopy, increasing the likelihood of detecting abnormalities and ensuring the procedure is both safe and effective.
15. Managing Anxiety and Stress
For many patients, anxiety is a natural response to the prospect of a colonoscopy. Discussing anxiety management strategies with your doctor beforehand can improve the experience and ensure cooperation during the procedure. Techniques may include mild sedation, breathing exercises, or calming conversations with the healthcare team.
Some patients benefit from bringing a support person or listening to music before the procedure to reduce stress. Addressing anxiety proactively allows patients to feel in control and reduces the psychological burden associated with medical tests. Doctors often emphasize that informed patients who understand each step of the process experience less fear and achieve better outcomes.
16. Transportation and Post-Procedure Safety
After sedation, patients are advised not to drive, operate machinery, or make important decisions for the rest of the day. Arranging transportation home and planning for post-procedure supervision is crucial. Patients should also be aware of dietary and activity recommendations for the remainder of the day, including consuming light meals and avoiding strenuous exercise.
Discussing these logistics with your doctor or care team ensures a smooth and safe recovery process. Patients who prepare in advance are less likely to experience complications or accidents after sedation, making planning an essential part of pre-procedure discussions.
17. Possible Complications and What to Watch For
Although colonoscopies are generally safe, potential complications exist, including bleeding, infection, or perforation of the colon wall. Patients should ask their doctor about warning signs that require immediate attention, such as severe abdominal pain, persistent vomiting, fever, or rectal bleeding after the procedure.
Knowing what to watch for allows patients to respond promptly to complications, ensuring timely medical intervention. Clear communication about risk factors and post-procedure monitoring empowers patients to manage their health effectively and reduces anxiety about rare adverse events.
18. Alternatives to Colonoscopy
While colonoscopy is considered the gold standard for colorectal screening, alternative options may be available depending on individual risk factors and medical history. These include stool-based tests, virtual colonoscopy (CT colonography), or flexible sigmoidoscopy.
Discussing alternatives with your doctor helps patients weigh convenience, comfort, and accuracy, and determine the best approach for their needs. Understanding options ensures that patients feel confident in their screening plan and are able to make informed decisions in consultation with their healthcare provider.
19. Frequency of Follow-Up Colonoscopies
After a colonoscopy, the need for follow-up depends on findings such as the presence of polyps, inflammation, or other abnormalities. Doctors may recommend more frequent surveillance for high-risk individuals or those with a history of polyps, while average-risk patients may return to routine intervals.
Clarifying follow-up frequency ensures that patients maintain appropriate screening schedules, reducing the likelihood of missed early detection. It also allows patients to plan ahead, manage insurance or coverage considerations, and stay engaged in long-term preventive care.
20. Comprehensive Conclusion: Empowering Patients Through Questions
The colonoscopy is a vital tool for early detection and prevention of colorectal disease, but its success depends on patient understanding and preparation. Asking the key question—“Why am I getting this colonoscopy?”—opens the door to a detailed conversation about risks, benefits, preparation, sedation, potential findings, follow-up, and alternatives.
By understanding every step, from bowel preparation to recovery, patients gain control over the experience and reduce anxiety. Knowledge about sedation, post-procedure care, complications, and frequency of follow-up ensures that patients are informed participants in their own healthcare.
Ultimately, a colonoscopy is not just a diagnostic procedure; it is a preventive measure that empowers individuals to take charge of their long-term health. Clear communication with your doctor, proactive questioning, and adherence to instructions maximize the effectiveness and safety of the procedure. Patients who approach colonoscopy with understanding and preparation benefit from early detection, reduced risk of colorectal disease, and peace of mind regarding their gastrointestinal health.
Conclusion
Colonoscopy is one of the most effective tools for maintaining digestive health and preventing colorectal diseases, including cancer. While the procedure may seem intimidating, understanding its purpose, preparation, risks, and benefits empowers patients to approach it with confidence. Asking the key question—“Why am I getting this colonoscopy?”—opens the door to an informed discussion with your doctor, ensuring clarity about your personal risk factors, expected outcomes, and follow-up care.
Preparation, including proper bowel cleansing, dietary adjustments, and planning for post-procedure recovery, plays a critical role in achieving accurate results and minimizing discomfort. Awareness of sedation options, potential findings such as polyps or inflammation, and the process of biopsies allows patients to anticipate each step and reduce anxiety. Furthermore, knowing the warning signs of complications, alternatives to the procedure, and long-term follow-up recommendations ensures proactive and responsible health management.
Ultimately, a colonoscopy is not merely a routine medical test—it is a preventive measure that can save lives. By approaching it with knowledge, preparation, and active engagement in discussions with healthcare providers, patients maximize the benefits while minimizing risks. Empowered patients are better equipped to make informed decisions, adhere to medical instructions, and take control of their gastrointestinal health. In summary, understanding every aspect of the colonoscopy, from why it is necessary to what to expect afterward, ensures a safer, more effective experience and strengthens long-term health outcomes.